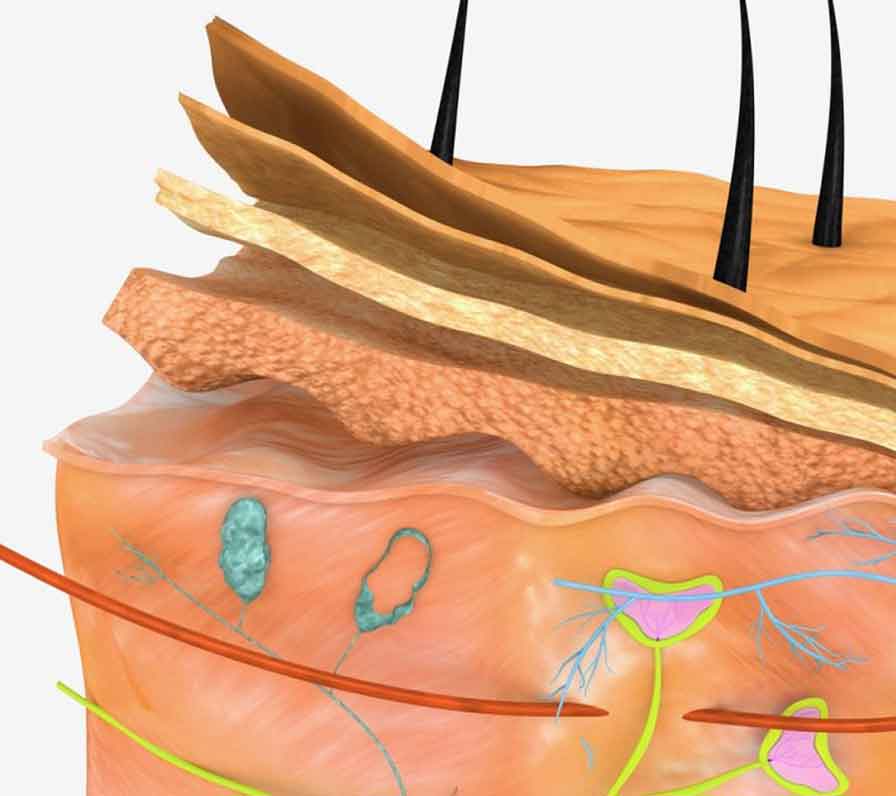
We all age one day at a time. So why do some people retain healthy-looking skin deep into adulthood, while others of the same age suffer wrinkles, lines, pigmentation, and other issues?
Part of the answer lies with genetics. Everyone’s skin ages the same way, but the rate at which skin ages can be vastly different from person to person. A significant part of the answer, though, lies with environmental factors. Sun exposure, personal habits, even sleeping conditions can cause the skin to put more energy into defending itself from external threats than into maintaining its youthful appearance, and can lead to prematurely aged skin.
This article will discuss several treatments for ageing skin. But first, we’ll take a look at the biological and environmental factors affecting our skin’s ageing process. Only with a complete view of these factors can a dermatologist recommend the right course of treatment for a given patient. You can learn about a professional’s perspective about noticible signs of ageing on the health portal UbiqiHealth. With that out of the way, here is the rest of the article!
How does skin age?
To get a clear view of what happens when skin ages, let’s start by considering skin at its youngest and see what changes over time.
Babies’ skin is so soft and smooth for two important reasons:
Secretions from the sebaceous and sudoriferous glands lubricate the epidermis or outer layer of the skin. Sebaceous glands secrete sebum, a substance made of fatty acids and waxes that quickly forms a thin film around a newborn’s skin, called the acid mantle. There it protects the skin from drying and offers some protection against bacteria. Sudoriferous glands produce sweat, which along with its cooling function brings moisture from the body to the skin, and helps keep it moisturized.
New skin cells arrive at a newborn’s epidermis every two weeks or so to replace cells that have died and naturally exfoliated. Soon, though, an infant body begins to retain some of those dead skin cells, which eventually form their own layer at the skin’s uppermost layer. This layer provides protection against external threats.
Over time, these benefits can become drawbacks. Sebum and sweat can attract dirt and encourage the development of harmful bacteria; once babies are out of swaddling clothes, this becomes increasingly likely. And their production, especially of sebum, is uneven as our bodies grow. Too much sebum can clog pores and ducts, leading to problems as we age.
Baby skin is also more elastic than older skin. Beneath the epidermis lies the dermis, which consists largely of a matrix of collagen fibres. Collagen is a strong, flexible protein that connects the epidermis to deeper tissues. Its most important job is literally keeping our skin in place; its other job is to lend shape and pliancy to our skin.
In babies, this layer is full of collagen, making skin appear smooth and free of wrinkles. As we age, we lose collagen, leaving skin less completely supported and more prone to wrinkles and sagging.
More subtle changes also affect the dermis. Capillaries—the tiny blood vessels lying close to the skin—can become constricted over time, leaving epidermal cells with less oxygen than they need. This can cause skin cells to die prematurely and can suppress the production of enough replacement cells. Eventually, what was once a protective layer of dead skin cells can become troublesome.
The sebaceous and sudoriferous glands can also come under attack. Overproduction of sebum and sweat can clog them, and a shrinking collagen matrix can reduce their size. This compromises the acid mantle, leaving skin cells more vulnerable to external threats. Particularly susceptible to these threats are the very organelles responsible for producing melanin; when these are damaged, irregular pigmentation often results, presenting itself as age spots.
What makes skin age prematurely?
Each person’s skin naturally ages the same way, though each is genetically predisposed to age at its own individual rate. Several external factors, though, have been shown to significantly affect the skin’s ageing process. To varying degrees, each of these is under each person’s control.
Stress and its impact on hormone production can add greatly to the ageing process. Stress can raise the body’s levels of testosterone, estrogen, and adrenocorticotropic hormones, sometimes with dramatic consequences for the skin. Hormones trigger events such as hair production and collagen replacement: the wrong message at the wrong time can greatly upset the body’s schedule.
Sun exposure is another widespread culprit. Most people are wise enough to apply sunscreen before spending long stretches of time outdoors on especially sunny days. But the types of radiation responsible for sun damage can penetrate clouds, and sunlight directed from reflective surfaces can be just as harmful as direct sunlight at the beach. Most people, even those who take proper care in obvious situations like sunbathing, simply get too much sun.
A given skin-care product may benefit the skin. But inconsistent or excessive of any product can be a bad idea, especially if that product has not undergone rigorous clinical analysis. Most new and unproven skin-care products contain some sort of biologically active ingredient, but without scientific proof of their effects in various scenarios, and without a carefully planned skin-care regimen surrounding them, many such products end up sending the skin a series of bewildering half-messages.
Even pillows can contribute to premature ageing: cotton-faced pillows can tug at the skin throughout the night. This might not be enough to wake anyone up, but it can keep the skin irritated just enough to contribute to premature ageing.
In response to each of these irritants and threats, skin reacts by limiting the extent to which it repairs damage and grows new tissue. This defensive response can have effects that show up immediately as signs of ageing.
What can be done about ageing skin?
With all of these threats to skin’s health, the best approach to prematurely ageing skin will differ greatly from person to person.
Chemical Peels
For many patients, chemical peels have long been the first (and sometimes the only) serious answer to ageing skin. Peels promise to remove the cuticle, or layer of dead skin cells, that often becomes unnecessarily thick as we age. While they do a good job at this, reducing the cuticle’s depth is only one part of the answer.
Peels have some advantages. They tend to deliver on what they promise: the removal of unnecessary skin cells and promotion of newer skin tissue. They are also relatively easy to perform and do not require the experience demanded of other procedures. This allows a wide range of aesthetic professionals, running from trained dermatologists to employees at beauty clinics, to competently perform peels of one kind or another. It also means that peels are widely available, and often at relatively affordable prices.
But on its own, a peel may provide short-term benefits while incurring long-term risks. We know that the causes of prematurely ageing skin can be numerous and complex. Without proper diagnosis and treatment of the true causes of a given patient’s skin condition, a peel simply opens the door to a solution the body isn’t prepared to provide.
If, for example, skin is poorly oxygenated because of constricted capillaries, new skin cells may not be healthy enough or be produced quickly enough, to take advantage of the opportunity given them by a peel. If the matrix of collagen supporting the epidermis has thinned greatly, a peel will not restore the firmness and shape once provided by the lost tissue.
Collagen Loss and Premature Ageing
No procedure—nothing available in a skin-care clinic or at a surgeon’s practice—can simply replace lost collagen or other components of the dermis. None can repair the fascia, the deep layer of collagen that connects the skin to bones and muscles. But some therapies can influence the dermis and its functions.
Transepidermal approaches, which work on the epidermis to influence the character and function of parts of the dermis, can improve nerve function, correct circulatory problems, and adjust the skin’s immune response. This last element is especially important: a healthy immune system doesn’t just fight disease, it helps identify dead and compromised skin cells themselves, and dispose of them properly.
Beneath the dermis, the fascia can also experience damage whose effects include visible signs of ageing all the way up at the epidermal layer. The facia is connected to the skin by bonds of elastin, a protein similar to collagen. Elastin, as its name suggests, is responsible for skin’s elasticity: its ability to return to its original state after moving. When the fascia is damaged, elastin works less effectively than it should, with predictable consequences.
The fascia is tougher material than collagen found elsewhere in the skin and is more resistant to damage. It is also more difficult to reach. Radio-frequency, LED, and electromagnetic treatments can reach the fascia and, similarly to the ways in which collagen is regenerated, encourage the body to produce more.
Because collagen, from the thinly woven strands near the epidermis to the tough fascia, is so important to the skin’s health and appearance, we’ll now look at two nonsurgical treatments for collagen loss.
Oral Treatments for Collagen Loss
Many types of collagen benefit from high levels of vitamin C, taken orally. The body can easily manage high levels of vitamin C and safely dispose of what’s needed, so regimens of more than 1,000 IU are often indicated to support collagen growth.
Sea buckthorn and evening primrose oil can also give the skin more of the materials it needs to produce more collagen. They also support the production of non-collagen tissues in the intracellular matrix, promoting fuller, smoother skin. These are often best used in conjunction with other types of treatment.
Topical Therapies for Collagen Loss
The market is crowded with topical creams and ointments promising to stimulate collagen growth. Many of them make claims that rest on tenuous observations and precious little clinically proven fact. Two compounds have been shown to encourage collagen growth: retinoids and ascorbic acid.
Retinoids are a group of compounds chemically similar to vitamin A, and like vitamin A they help to regulate cell growth. Because they work at such a fundamental level, retinoids can have unintended consequences if prescribed incorrectly or taken excessively. Taken with care, though, they can be directly responsible for the creation of new fibroblasts that create collagen and elastin.
As we age, our body produces fewer fibroblasts to replace those that have died. This is the functional reason why we produce less collagen and elastin. Retinoids augment the body’s waning interest in creating new cells, including the fibroblasts that produce collagen.
Ascorbic acid, or vitamin C, works one level above that of retinoids. While retinoids encourage the creation of new fibroblasts, ascorbic acid is responsible for fibroblasts’ function. Provided enough of the correct amino acids, any fibroblast in the extracellular matrix can produce collagen. But it needs to be told to do so.
Ascorbic acid delivers that message. When chemically triggered by ascorbic acid, collagen-producing fibroblasts create tropocollagen, a collagen precursor, around a peptide. They then add to this precursor before a complete collagen molecule is produced. After bonding several collagen molecules into a strand, the fibroblast releases the finished product into the matrix, where it soon finds a home.
Administered together, retinoids and ascorbic acid can give skin the building blocks and the instructions it needs to regenerate collagen at a higher rate.
pH and Ageing Skin
The skin’s pH level—its acidity or alkalinity—also affects its appearance, and may contribute to premature ageing.
The acid mantle that protects the skin of newborns may require some pH adjustment in later life. When the beneficial layer of dead skin cells that forms on mature skin becomes too thick, high pH may be the culprit. When the skin’s surface is too alkaline, dead skin cells bond together just enough to stay in place, rather than flaking off. Lowering the skin’s pH level hardens this layer and makes it more brittle, allowing cells to fly off naturally.
Skin that is prone to acne may benefit from an abrupt increase in alkalinity. Ph levels above 12 inhibit the growth of bacteria, both good and bad. Raising the skin’s alkalinity, even temporarily, can kill all protein-based cells, including bacteria, dead skin cells, certain kinds of scar tissue, and even organisms that cause rosacea.
Any agent capable of quickly raising or lowering pH should be applied carefully, by an experienced hand. Improper application of such products can lead to the destruction of healthy skin tissue. In any case, the skin’s pH should be neutralized immediately after treatment and allowed to return to its normal pH level.
Other Topical Therapies for Ageing Skin
A combination of proven enzymes like papain can address the ageing effects of dead skin cells. Combined with dermal fillers, these topical applications can improve the appearance of the skin’s surface layers while supporting the underlying dermis.
Another approach to removing dead skin cells addresses their adhesive properties. Dead cells include a natural cement that binds them together. In babies and young children, this cement is routinely dissolved by the epidermis, and dead cells are free to leave. In adults, this process slows, contributing to dead skin cells’ tendency to remain on the body.
Alpha hydroxy acids can safely dissolve this cellular cement when used correctly but can cause problems including inflammation if overused. Glucolic acid is the alpha hydroxy acid most commonly used for exfoliation; it penetrates so readily into deeper layers of the skin that it is also recommended for hyperpigmentation issues, and may even encourage collagen growth. Other alpha hydroxies include lactic, mandelic, and citric acids.
Skin can age prematurely for dozens of reasons, and for each cause of ageing skin, there are several proven remedies. Only a consultation with an experienced dermatologist can identify the treatment—or, more commonly, the group of treatments—best suited to a given patient.